Case Study: Designing an app to reassure those who care about a loved one with dementia
Is the answer already in their wi-fi?
One million people in the UK will have dementia by 2025 which is a predicted rise of 35%. (Prince, M et al, 2014)
In a team of five UXers, we investigated ways Internet of Things data could be used to help prolong ‘aging in place’ for people in the early stages of dementia. While technology cannot replace seeing and caring about someone in person, we found there was a way to provide reassurance for their loved ones, when they can't be with them in person.
Our process
Researching the context
Worldwide, around 50 million people have dementia, with nearly 60% living in low and middle-income countries (World Health Organisation, 2020). Every year, there are nearly 10 million new cases. The estimated proportion of the general population aged 60 and over with dementia at a given time is between 5-8%. One million people in the UK will have dementia by 2025 (Prince, M et al, 2014) which is a predicted rise of 35%.
Promoting 'aging in place' may help our ageing population to remain living safely and independently in their own home or community for longer. We propose a system aiming to promote an independent lifestyle for people in the early stages of dementia, with mild cognitive impairment. Our aim is to create an unintrusive system which makes use of existing devices in the home and sensor technology.
There are other systems already on the market that use similar technology. Typically, these focus on providing surveillance data to caregivers rather than directly assisting the PwD. Another system, the TV-AssistDem provides a model that is more based around connecting patients with medical care and advice. While advances in telemedicine would help this model, our model is looking more at aiding with daily life and reassurance for caregivers.
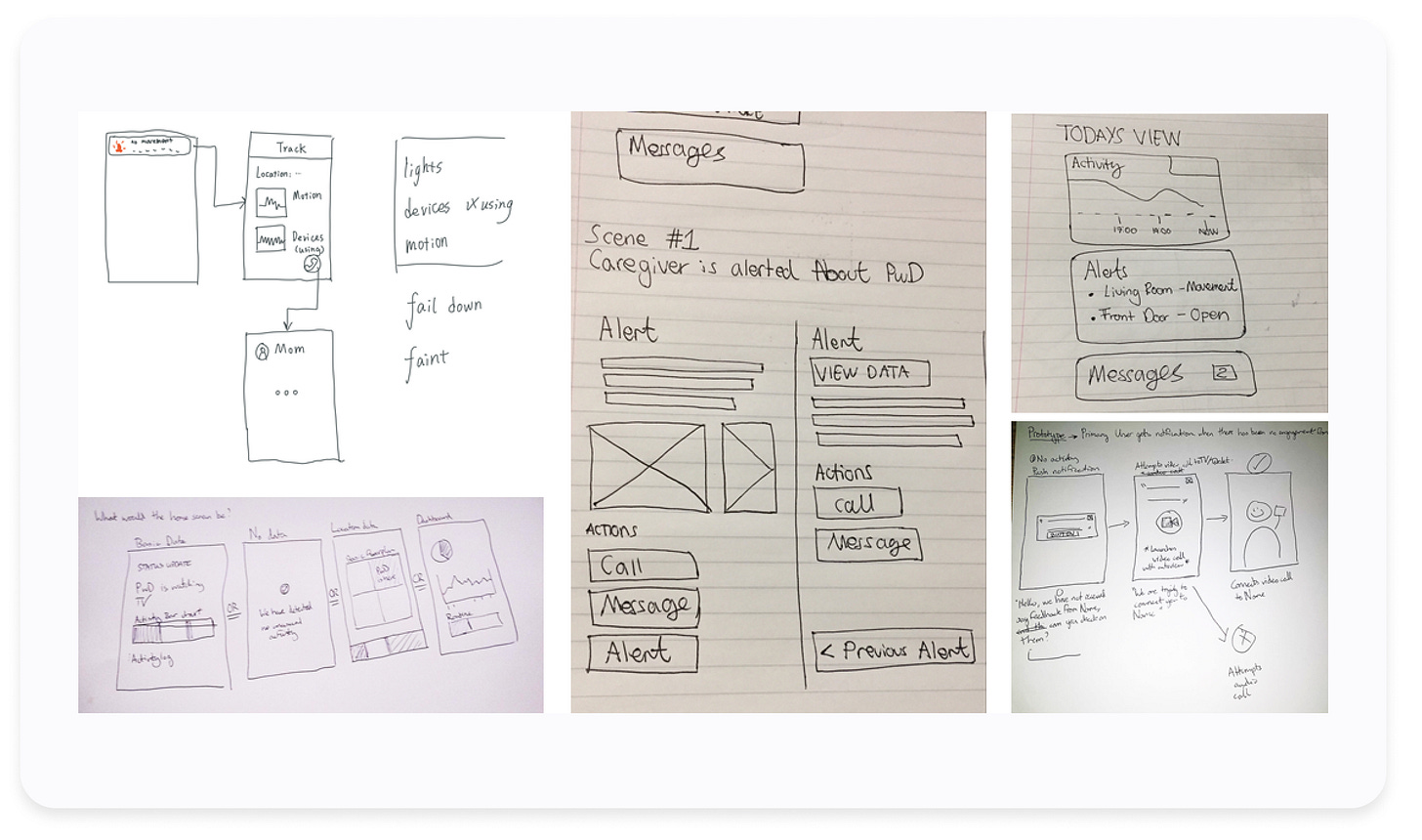
Sketching out solutions
Through a series of collaborative design workshops, we discussed what we wanted to create and sketched out different options of how we could display the data to make it useful. We also considered various technologies – could the product use AI to identify behavioural patterns? Were we designing a system that with communications channels?
It was at this point in the process we first wanted to bring our primary user group in, to make sure we were creating something useful.
Asking the users
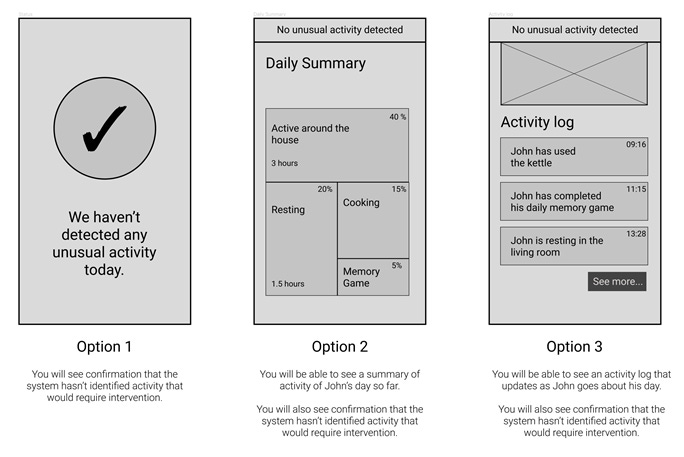
We decided on three low-fidelity dashboards with varying levels of content to put in front of the users. These were used as a prompt to address privacy issues we’d identified and find out what people want to see.
“Less information would still make me wonder.”
Our users told us they understand the routine of their loved one so they want to be able to see all the info – both for reassurance and if they could see something unusual. When asked which option the person they are caring for would want them to see, our users were more divided. What was clear is that users would not trust a system to make decisions on what was usual on their behalf.
Based on the feedback from our users, we took it back into design and began plotting out our user flow:
My design challenge
After speaking to our users, we realised that the majority wanted to know as much information as possible. This raised ethical concerns with how we can give them just enough home activity data that they felt reassured, without infringing on the privacy of the person with dementia.
Understanding from our background research the intricacies of the condition and how it affects everyone differently, we also needed to ensure our product could be personalised to that family's situation.
To tackle this, I designed a feature that lets users set an alert when a routine device is activated to let our users know things are happening as normal. This gets around users having access to all the information and encourages them to think about what they need to know to feel reassured.